candrew
Well-Known Member
View attachment 9208
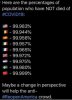
Someone I know shared this on Facebook. For me, it's brushing people who've died under the rug.
Thoughts?
@One Brow @Zombie
You guys are pretty informed.
If anything this speaks to the absolute **** show that we're currently living in. People get sick, go to the hospital and die and are never confirmed as having Covid-19 because there aren't enough diagnostic tests. So it becomes a guessing game for the doctor who fills out the death certificate. Some put Covid-19, others pneumonia. But before you start marching in the streets without a mask on take a look at these numbers:
Deaths attributed to pneumonia this year:
New York - up 651%
New Jersey - up 670%
Michigan - up 172%
These numbers speak for themselves.
It also bears mentioning that, historically, the true number of people who die during a pandemic are typically underreported during the infection period. For example deaths attributed to the swine flu in 2009 were initially reported at about 20 thousand - a study done three years later put the number of deaths at close to 285 thousand.
I think something worth investigating is why is the richest country in the world currently 42nd in Covid-19 testing per capita.